
For decades, people with lower back pain were often told there was only one real solution to their misery: Spinal fusion, in which two or more bony vertebrae are surgically ''welded" together in hopes of reducing pain and stabilizing the back.
The trouble is, there has never been compelling evidence that this works well, partly because new problems occur, like stiffness and increased pressure above and below the fused vertebrae. And the risks of fusion surgery are serious -- bleeding to the point of needing a transfusion, and accidental nerve injury, leading to pain or weakness.
Happily, two developments are increasing the options for the millions of us with aching backs: potentially better surgery, and a new attitude toward exercise.
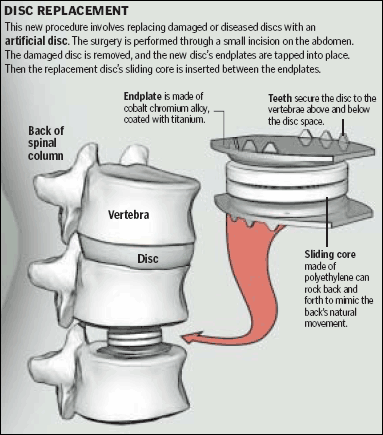 Late last fall, the US Food and Drug Administration approved the first
artificial disc, called Charite. This plastic and metal disc, made by a
Late last fall, the US Food and Drug Administration approved the first
artificial disc, called Charite. This plastic and metal disc, made by a
So far, about 1,000 US surgeons have started doing this surgery, said Dr. Rick Delamarter, medical director of the Spine Institute at St. John's Hospital in Santa Monica, Calif. Though there's little long-term data, early results suggest it may be equivalent to fusion for pain reduction but allow for a quicker recovery, more flexibility, and fewer problems in adjacent areas of the spine.
There is also growing evidence that many people do not need surgery at all. In 2001, a landmark Swedish study showed that while fusion did decrease pain over the first two years -- by 33 percent compared with a 7 percent reduction in pain for those who didn't have surgery -- no differences were noted in the long run, according to follow-up data.
In 2003, a Norwegian study showed that an aggressive exercise program plus cognitive behavior therapy reduced pain just as much as fusion after the first year. (One key was teaching people that, contrary to their fears, it is safe to be physically active despite pain.) And a still-unpublished English study found similar results.
Taken together, the three studies ''show little or no advantage of fusion. After five to 10 years, everybody looks pretty much the same. The folks without surgery gradually get better on their own and the ones who do have surgery have faster improvement but gradually have back pain again," said Dr. Richard Deyo, director of the multidisciplinary research center on spinal disorders at the University of Washington in Seattle.
''The trouble is," he said, ''American surgeons don't believe these results."
In 2002, the latest year for which figures are available, 293,000 Americans had fusion surgery, according to the North American Spine Society, and the numbers have been rising every year. The operation is lucrative, not just for surgeons and hospitals, but for companies that make the special screws and ''cages" to hold vertebrae together. The hardware alone can cost $5,000 to tens of thousands for one operation.
And many respected surgeons genuinely swear by the procedure, among them Dr. Richard Guyer of the Texas Back Institute, who said that 75 to 80 percent of people who have the operation say it helped them.
But the tide seems to be turning away from fusion surgery.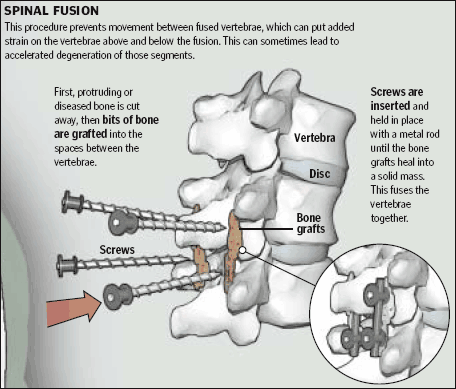
This week in New York City, 1,000 spine surgeons are expected to discuss the new artificial discs and other non-fusion approaches at a meeting of the Spine Arthroplasty Society. ''Non-fusion technologies such as artificial discs represent a paradigm shift in the surgical treatment of degenerative spine problems," said Dr. Frank Cammisa, chief of spinal surgery at the Hospital for Special Surgery in New York, and chairman of the meeting.
Some kind of surgery remains necessary when there is a loss of bladder or bowel control, progressive weakness in the legs, paralysis, and pain that shoots down the leg (sciatica) and doesn't get better over time. Surgery may also be necessary with spinal stenosis, in which the spinal canal, through which the spinal cord passes, narrows from arthritis.
But most people with lower back problems should ''aggressively pursue exercise and nonsurgical approaches before turning to surgery," said Dr. David Matusz, a spine surgeon at Johns Hopkins Medical Center.
This ''conservative" therapy can also include rest and ice for a few days during the acute attack, then acupuncture, physical therapy, chiropractic, anti-inflammatory drugs like Advil or Aleve, and cortisone injections.
It's not clear even at a basic physiologic level that surgery is the right approach to lower back pain, said Dr. James Rainville, chief of physical medicine and rehabilitation at New England Baptist Hospital in Boston. The simplistic assumption is that lower back pain is caused by disc problems. But pain is actually a neurological phenomenon that ''is not occurring solely in the spinal structures associated with movements."
When a person feels acute back pain, the central nervous system goes into high gear, becoming ''sensitized," meaning that nerves become hyperactive, turning acute pain into chronic pain. Once chronic pain sets in, any little movement can be excruciating.
What exercise and cognitive behavioral therapy can do -- and surgery does not -- is re-train the brain and the rest of the nervous system to become less sensitive, Rainville said, allowing the feeling of pain to gradually go away.
So what should you make of all this if you have persistent lower back pain? First of all, recognize that some back problems are inevitable. Disc degeneration from wear and tear is universal with aging, though much of the time, this doesn't cause pain and even when it does, usually goes away on its own. ''Bulging" discs, in which the disc pokes out and may press on a nerve, are also common, and are sometimes called herniated or slipped discs. They, too, often get better on their own.
If, despite aggressive nonsurgical approaches, you still have chronic lower back pain, especially pain running down the leg that persists for several months, and if a CT or MRI scan shows that you have a disc or part of the vertebra pressing on a nerve, try to have the least invasive surgery possible.
This includes discectomy for relief of leg pain -- removing just the troublesome disc or part of it, or possibly getting an artificial disc if the main problem is back pain. Bear in mind, though, that there's still relatively little data on artificial discs, and doctors don't have much experience with it. You can also consider a laminectomy, in which part of the bony vertebra is removed to relieve pressure on a nerve that causes leg pain.
As a last resort, there is spinal fusion. But if you're going this route, get
a second opinion to be sure the operation is truly necessary and likely to help
you. ![]()
original article posted at http://www.boston.com/yourlife/health/fitness/articles/2005/05/03/aching_spines/